IVF

One of the options available to our patients seeking to conceive is in vitro fertilization (IVF). This Assisted Reproductive Technology (ART) is a common and highly-successful treatment option. The four basic principles of IVF are 1) stimulating the ovaries to produce more than one egg 2) removing the eggs from the ovaries, 3) fertilizing the eggs in the laboratory and 4) placing the embryo(s) into the uterus for implantation.
Ovarian Stimulation
In nature, a single egg (also called an oocyte) is released from the ovary monthly, then waits to be fertilized. In vitro fertilization is more effective when multiple eggs are available at the time of retrieval. For this reason, injectable fertility medications are used to stimulate the follicles to produce more than one egg in a cycle. For more information on fertility medication, visit our Resources page.
Egg Retrieval
The egg retrieval process is a minor outpatient surgery performed at CARE for the Bay Area. To remove the eggs from the ovary, a hollow needle is inserted directly into each follicle. The physician uses ultrasound technology to locate the follicles, then the liquid which surrounds each egg is sucked out (“aspirated”). The fluid is given to the Embryologist in the laboratory where the egg is isolated away from the fluid and placed in a petri dish for fertilization.

Fertilization
While the patient undergoes the egg retrieval procedure, the male partner provides a semen sample. This sample is delivered to the laboratory where it is processed (“washed”). The retrieved eggs are placed in a petri dish in a special solution designed to provide all the necessary nutrients for growth and fertilization. The sperm and eggs are incubated together and after 16-18 hours, the eggs are examined by an embryologist. This procedure is known as conventional IVF.
In cases of severe male infertility, a procedure known as intra-cytoplasmic sperm injection (ICSI) is used. In ICSI cases, a single sperm is directly injected into each egg. Fertilization is again assessed after 16-18 hours.
Embryo Transfer
An embryo is created following the successful fertilization of an egg. The embryos are maintained in the laboratory for several days prior to being replaced in the body. Embryos may be transferred back into the uterus following culture for 3 days in the laboratory. Alternatively, a blastocyst transfer may be indicated by your physician; in these instances, the embryos will be cultured for 5-6 days. The laboratory uses several embryo characteristics to determine which embryos are best (high-quality) for transfer. The embryo transfer is a simple procedure which does not require anesthesia. The selected embryo(s) are inserted into a thin tube called a catheter that is guided into the patient’s uterus.
Additional advanced fertility treatments
There are several additional advanced fertility treatment options available to our patients. These include embryo freezing of additional high quality embryos not selected for transfer, pre-implantation genetic screening (PGS) for chromosomal abnormalities, pre-implantation genetic diagnosis (PGD) for disease or mutation carriers, and assisted hatching.
Embryo Freezing
Patients may have additional high-quality embryos that are not chosen for embryo transfer. These embryos may be frozen for the patient’s future use in a frozen embryo transfer (FET). Use of cryopreserved (frozen) embryos avoids the need for repeat stimulation and retrieval since these embryos have already been created. Embryo cryopreservation can optimize success rates, decrease multiple pregnancies, decrease costs of future treatment as well as prevent embryo waste.
Pre-implantation genetic testing of Aneupoloidy(PGT-A)
Pre-implantation genetic testing for aneuploidy (PGT-A) can be used to identify chromosomal abnormalities or “aneuploidies” in embryos created by IVF. By avoiding transfer of aneuploidy embryos, the risk for pregnancy failure is reduced and the probability of conceiving a viable pregnancy is improved. For more information, please see our PGT section.
Pre-implantation genetic testing for single gene defects and structural rearrangement(PGT-M/PGT-SR)
Pre-implantation genetic testing (PGT) allows embryos developed via IVF to be screened for genetic disorders. This is particularly useful for patients who are at risk for passing on inherited genetic disorders such as cystic fibrosis or muscular dystrophy. For more information on this powerful tool, please see our PGT section.
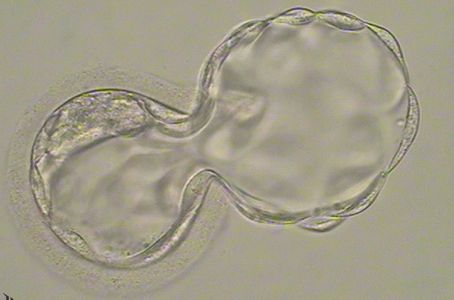
Assisted Hatching
To achieve pregnancy, an embryo must implant into the wall of the uterus. Prior to implanting, the embryo “hatches” from its hard outer covering. For some patients, the embryo is unable to “hatch” on its own. In these instances, assisted hatching can be performed to increase the patient’s chances of conceiving.
Copyright © 2020 C.A.R.E. for the Bay Area - All Rights Reserved.
Powered by GoDaddy
